You didn't notice it the first week. By month three it wakes you at night. This is the exact escalation pattern of overhead shoulder damage — and why ignoring it costs you years, not days.
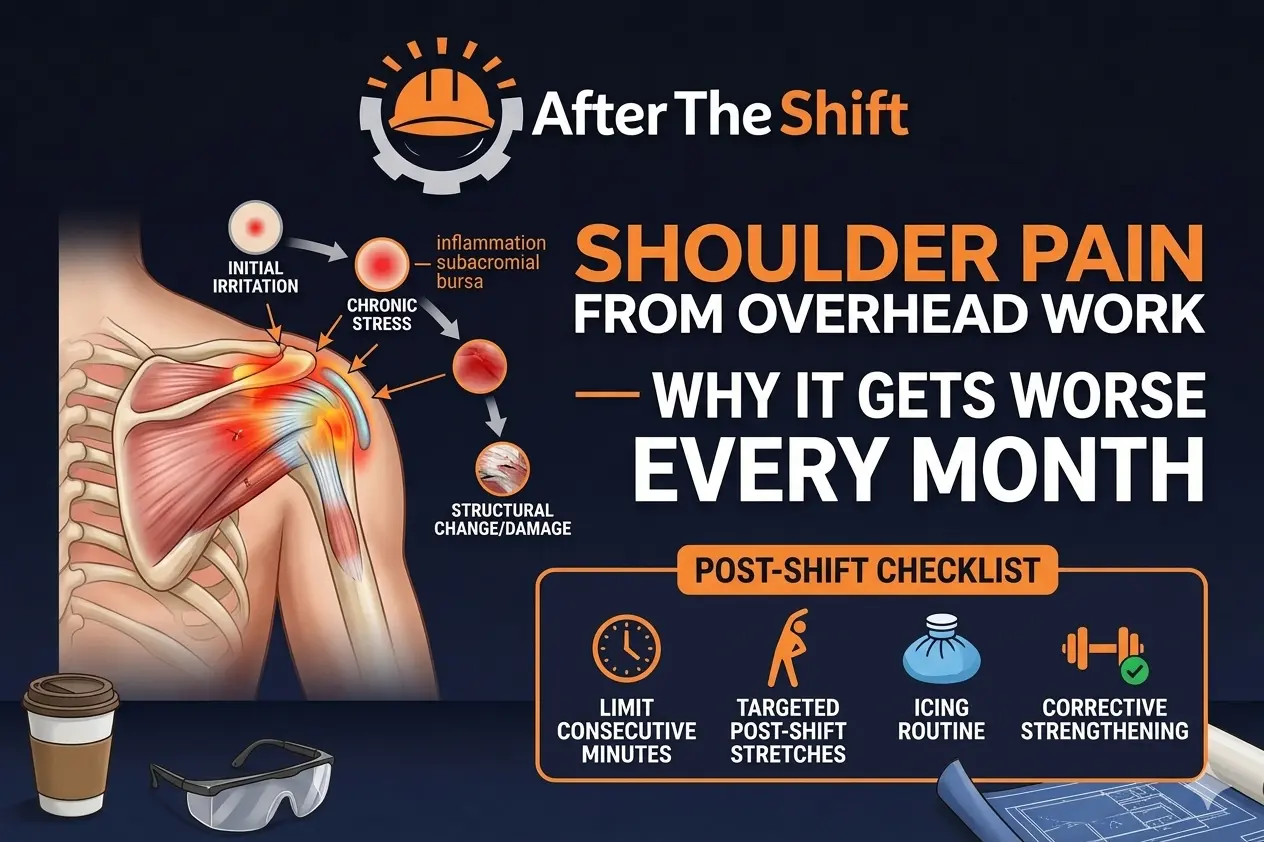
Shoulder Pain from Overhead Work — Why It Gets Worse Every Month
You didn't notice it the first week. By month three it wakes you at night. This is the exact escalation pattern of overhead shoulder damage — and why ignoring it costs you years, not days.
Quick Answer
Overhead work loads the rotator cuff and bursa in a way that doesn't fully heal between shifts. Damage compounds. If it hurts during the shift now, it will hurt at rest within 3–6 months without intervention.
- Do: Drop arms below shoulder height for 2–3 minutes every 20 minutes on-shift
- Do: Decompress the shoulder (arm hang, doorway stretch) after every shift
- Do: Get a physio assessment if pain has lasted more than 4–6 weeks
- Avoid: Sleeping on the affected side
- Avoid: Using ibuprofen daily to keep working — it masks the signal, not the damage
- Red flag: Pain at rest, weakness lifting the arm, or arm numbness = stop overhead work and get checked
- Timeline: Stage 1–2 responds to rest + rehab in 4–8 weeks; Stage 3–4 may need 3–6 months or surgery
In This Article
- What's Actually Happening Inside Your Shoulder
- The Monthly Escalation Pattern
- Symptom → Cause → Fix Matrix
- How Bad Is It Right Now? (Decision Tree)
- The 4 Damage Stages
- Score Your Shoulder Risk (Mini-Test)
- What Actually Helps — and What Makes It Worse
- Treatment Options Compared
- Mistakes That Speed Up Damage
- FAQs
- What to Do Next
What's Actually Happening Inside Your Shoulder
The shoulder is the most mobile joint in the body — which also makes it the least stable. When you work overhead — painting ceilings, installing conduit, stacking high shelves, roofing, strapping loads from above — you're repeatedly loading a joint that was never designed for sustained force above shoulder height.
There are two main structures that take the hit in overhead work:
- The rotator cuff — four muscles that hold the humeral head centred in the socket. Repeated overhead loading stretches and tears these fibres microscopically. Full repair takes 48+ hours. If you're doing overhead work five days a week, the fibres never get it.
- The subacromial bursa — a fluid-filled sac that prevents friction between the cuff and the acromion bone above it. Overhead work compresses this sac thousands of times per shift. Over weeks, it becomes chronically inflamed (bursitis), and the space it sits in shrinks — causing impingement each time you raise your arm.
The reason it gets worse every month: each shift adds micro-damage that slightly exceeds what the tissue can repair overnight. The deficit compounds. What begins as fatigue becomes inflammation, which becomes structural change. This pattern is explained in detail in our guide to how micro-damage destroys joints silently.
The blunt rule: If your shoulder hurts during the shift — not just after — you are past the fatigue stage. You have active tissue damage. Every day you continue without changing something adds to a deficit that will not reverse on its own.
The Monthly Escalation Pattern
Most overhead workers describe the same trajectory. It doesn't happen in days — it happens over months, which is exactly why it bypasses every warning your brain should be raising.
| Timeframe | What You Feel | What's Actually Happening | Typical Mistake |
|---|---|---|---|
| Week 1–4 | Soreness after shifts, gone by morning | Muscle fatigue, minor bursa irritation | "I'll sleep it off" — and it works, temporarily |
| Month 1–2 | Still sore after shifts; takes a full day off to clear | Bursa beginning to inflame; cuff fibres accumulating micro-tears | "It's just part of the job" — adaptation myth kicks in |
| Month 2–4 | Pain during the shift; aches at night; stiff in the morning | Chronic bursitis; early impingement — subacromial space narrowing | Ibuprofen to keep working — masks pain, doesn't stop damage |
| Month 4–6 | Wakes you at night; reaching behind the back is difficult | Partial rotator cuff tear likely; frozen shoulder risk rising | Waiting for it to "settle down" — it won't without treatment |
| 6+ months | Constant pain; significant strength loss; restricted motion | Full-thickness tear or adhesive capsulitis — surgical territory | "I can't afford time off" — until they have no choice |
The critical window is months 1–3. That's when damage is still largely soft-tissue and responds to rest, physio, and load modification. After month 4–5, the odds of needing injections or surgery climb sharply. Read more about the too-late line physical workers don't see coming.
Symptom → Cause → Fix Matrix
Not all shoulder pain is the same. Match your symptom pattern to the most likely cause and the correct first step. Getting this wrong — especially treating a tear as plain bursitis — wastes weeks and worsens the outcome.
| Symptom | Most Likely Cause | First Fix Step | Red Flag? |
|---|---|---|---|
| Ache at end of shift, gone next morning | Muscle fatigue, minor bursa irritation | Decompression stretches; reduce overhead hours | No |
| Pain at front/top of shoulder during overhead lift (painful arc 60–120°) | Subacromial impingement or bursitis | Avoid overhead 2 weeks; ice after shifts; book physio | If not improving in 2 weeks, yes |
| Pain wakes you when you roll onto the shoulder | Bursitis + possible early rotator cuff tear | See a physio this week — conservative treatment window closing | Yes |
| Weak arm — can't lift to shoulder height or resist light pressure sideways | Partial or full rotator cuff tear | Stop overhead work immediately; get ultrasound or MRI | Yes — urgent |
| Stiffness and loss of rotation — can't reach behind back or across chest | Adhesive capsulitis (frozen shoulder) forming | Physio immediately — the longer you wait, the longer it takes to unfreeze | Yes |
| Clicking or grinding with no pain | Scapular muscle imbalance; minor labrum irritation | Posterior shoulder strengthening: face pulls, band pull-aparts | Not yet — monitor |
| Pain radiating down arm to elbow or hand; pins and needles | Cervical nerve root or thoracic outlet syndrome — not primarily the shoulder | See a doctor before starting shoulder rehab — wrong treatment causes harm here | Yes — different issue |
| Pain only when reaching behind the back | Subscapularis strain or posterior impingement | Cross-body stretches; avoid reaching behind with a load | 2 weeks no improvement → physio |
How Bad Is It Right Now? (Decision Tree)
Follow the branches. This routes you to the correct action without guesswork.
├── YES → Is it constant or does it come and go?
├── Constant → Can you lift your arm to shoulder height against resistance?
├── No / Very weak → Stop work. Get imaging this week. Likely partial or full tear.
└── Yes, strength intact → Active bursitis or Stage 3 impingement. Physio this week, not next month.
└── Comes and goes → Is it worse at night lying on it?
├── Yes → Early-to-mid bursitis. Start physio, sleep on the other side. Do not keep pushing overhead.
└── No → Apply the decompression and load reduction protocol below. Review in 2 weeks.
└── NO → Does it hurt only when working overhead?
├── YES → How long has this been happening?
├── Under 4 weeks → Early fatigue/irritation window. Load reduction + decompression now. This is the cheapest fix point.
└── Over 4 weeks → Developing impingement. Book physio now — don't wait for it to worsen.
└── NO → Sore only after the shift?
├── Yes → Normal load fatigue. Start the post-shift decompression routine tonight.
└── No pain → You're ahead of it. Build protective habits now — 10 minutes/day costs nothing; Stage 3 costs months.
- Numbness or tingling running down the arm
- Sudden sharp pop followed by immediate weakness
- Cannot raise the arm above 90 degrees
- Pain does not ease after 2 full days off work
- The shoulder looks visibly different or swollen compared to the other side
The 4 Damage Stages of Overhead Shoulder Injury
Not everyone progresses through all four — but this is the typical arc when overhead damage goes unaddressed. Knowing your stage determines your treatment window, your recovery timeline, and whether you still have non-surgical options.
| Stage | What You Feel | What's Damaged | Recovery Time | Action Required |
|---|---|---|---|---|
| Stage 1 Fatigue/Irritation |
Post-shift ache; clears overnight | Muscle fatigue; minor bursa irritation | 1–2 weeks rest + decompression | Load management; arm-hang post-shift; posterior shoulder work |
| Stage 2 Impingement |
Pain during overhead movement; lingers post-shift | Chronic bursitis; subacromial space narrowing | 4–8 weeks with physio | Physio 2x/week; reduce overhead load 60%+; external rotation rehab |
| Stage 3 Partial Tear |
Night pain; weakness; pain at rest | Partial rotator cuff tear — supraspinatus most common | 3–6 months; possible injection | Imaging; physio or steroid injection; no overhead work |
| Stage 4 Full Tear / Frozen |
Significant ROM loss; severe weakness; constant pain | Full-thickness tear or adhesive capsulitis | 6–18 months; often surgery | Orthopaedic referral; surgical assessment likely needed |
Stage 1 and early Stage 2 intervention costs you two weeks and €0–80 in physio. Stage 3 and 4 can cost you six months of income and potentially your ability to stay in a physical trade. The gap between these outcomes is almost always just how long you waited. See why toughing it out makes injuries worse.
Score Your Shoulder Risk (Mini-Test)
Check every box that applies to you. Each one scores 1 point. Your total determines the action level.
What Actually Helps — and What Makes It Worse
Most workers either do nothing or do the wrong thing. Both approaches extend the injury timeline. Here's the split — the right column is where most of the damage accumulation happens.
| ✓ Helps | ✗ Makes It Worse |
|---|---|
| Passive arm hang (60 seconds) — decompresses the subacromial space post-shift | Sleeping on the affected shoulder — compresses the bursa for 6–8 hours |
| Ice pack 15 minutes after work during acute flare-up | Daily NSAIDs without load reduction — masks the signal, doesn't stop the damage |
| Posterior shoulder strengthening: face pulls, band pull-aparts, rear delt rows | Pressing exercises (bench press, shoulder press) when the bursa is already inflamed |
| Sleeper stretch and cross-body arm stretch for posterior capsule tightness | Aggressive stretching during an acute inflammatory flare — makes bursitis worse |
| Arms-down break every 20 minutes during overhead tasks — drops intra-bursal pressure | Pushing through pain to finish the job — each time you do this, you add days to recovery |
| Physio-directed external rotation strengthening — the most evidence-backed rehab for impingement | Generic YouTube shoulder workouts without knowing your stage — wrong protocol for your tissue state |
| Scapular retraction during overhead tasks — keeps the subacromial space open | Ignoring the other shoulder — compensatory overloading the "good" side creates a second injury |
Treatment Options Compared
| Treatment | Best For | Skip If | Cost / Timeframe |
|---|---|---|---|
| Load reduction + self-rehab | Stage 1, early Stage 2 | You have weakness — needs diagnosis first | Free; 2–4 weeks |
| Physiotherapy | Stage 2–3; all stages benefit from proper assessment | Stage 4 full tear without surgical clearance | €40–80/session; 6–12 sessions typical |
| Corticosteroid injection | Acute bursitis; Stage 2–3 where physio has stalled | More than 3 total — tendon tissue weakens with repeated injections | €100–200; effect lasts weeks to months |
| Imaging (ultrasound / MRI) | Stage 3–4; any suspected tear; no improvement after 6 weeks of physio | Not an avoidance — get it when the stage warrants it | Ultrasound €80–150; MRI €200–500 |
| Arthroscopic surgery | Full-thickness tears; failed conservative treatment after 3–6 months | Stage 1–2 — surgery is not the first answer for overhead impingement | 6–12 month recovery; significant income and time cost |
Mistakes That Speed Up Damage
These aren't rare errors. Every one of them gets made on job sites every week.
- Waiting for it to go away on its own. Stage 1 sometimes does. Stage 2 never will. Most workers who end up in surgery waited 3–6 months past the point where physio would have fixed it. The injury didn't fail them — the delay did.
- Using ibuprofen as a work permit. NSAIDs reduce the pain signal, not the structural damage. You can now do more damage without feeling it. This is not a strategy — it's borrowing from your future self at very high interest.
- Resting completely without any rehab. Complete rest without active rehabilitation lets the shoulder stiffen. This is one of the main accelerators from Stage 2 impingement to Stage 4 frozen shoulder. Movement within a pain-free range is essential.
- Only stretching the front of the shoulder. Most overhead workers have a tight anterior capsule and weak posterior cuff — the typical imbalance from forward-arm repetitive work. Stretching only the front worsens the very imbalance that caused the impingement.
- Ignoring posture during overhead tasks. Arms wide, shoulders shrugged, neck forward — this maximises impingement. Keeping elbows closer to the body and retracting the shoulder blades before and during overhead work measurably reduces subacromial compression.
- Writing it off as "just age." Most overhead shoulder damage in physical workers is load accumulation — not age. Stage 3 injuries happen at 24 in roofers and electricians. Age doesn't cause this. Unmanaged overhead volume does — and that's something you can actually change.
FAQs
▸ Can I keep working overhead while my shoulder heals?
It depends entirely on the stage. Stage 1: yes — reduce overhead hours, rotate tasks, and take arms-down breaks every 20 minutes. Stage 2: only if overhead time is cut by at least 50–60% and you are actively in physio. Stage 3+: continuing overhead work without medical clearance will worsen the tear with every shift. If it hurts during the job, you are compounding damage — not getting through it.
▸ How do I tell if it's bursitis or a rotator cuff tear?
You can't reliably tell from symptoms alone — they overlap heavily. The clearest indicator of a tear versus pure bursitis is weakness: if you cannot hold your arm up against light resistance, or the arm drops when attempting to lift it to the side, suspect a tear. A physiotherapist can differentiate with clinical tests (Empty Can, Hawkins-Kennedy, external rotation lag). Ultrasound confirms it. Don't self-diagnose as "just bursitis" and follow bursitis rehab if you have actual weakness — the treatment approach is different.
▸ I've had this for 8 months. Is physio still worth trying?
Yes — physio can still be effective at 8 months, but the process is slower and the outcome less predictable. Partial tears treated conservatively at 8 months can still recover without surgery, but it takes 3–4 months of consistent rehab. The key variable is whether there's a full-thickness tear, which needs imaging to confirm. At 8 months with no improvement: get an ultrasound first, then begin structured physiotherapy based on what the scan shows.
▸ Will a steroid injection fix the shoulder?
A corticosteroid injection reduces inflammation and can give significant pain relief for weeks to months — but it does not repair damaged tissue. For bursitis, it can break the inflammatory cycle long enough for physio to take hold. For a tear, it reduces pain but the structural problem remains. It's a bridge, not a cure. If you get an injection and feel better, that's the window to do your physio and modify your workload — not to return to full overhead hours.
▸ My shoulder only hurts on one specific movement. Is that less serious?
Movement-specific pain is actually useful — it often points to a specific structure, which makes treatment more targeted. Pain on the painful arc (60–120° of elevation) = impingement. Pain at the very top of the arc = acromioclavicular joint. Pain reaching behind the back = subscapularis or posterior impingement. The risk with "it's only one movement" thinking is complacency. Movement-specific pain at Stage 1–2 is far easier to resolve than diffuse, constant pain at Stage 3. Don't wait until it spreads.
▸ Will two weeks off work fix it?
Stage 1 irritation: often yes — two weeks off can reset it almost completely. Stage 2 bursitis: partial improvement, but without addressing the mechanical cause (muscle imbalance, overhead technique, posture), it returns within days of going back to the same work. Stage 3+: rest alone will not fix structural damage. You need active rehabilitation, not just absence. Time off helps manage symptoms; it does not reverse tissue damage.
▸ I'm 23. Can I already have a rotator cuff tear?
Yes. Rotator cuff tears are not an older person's injury. In physical workers doing high-volume overhead tasks, partial tears from ages 18–30 are well documented — particularly in roofers, electricians, and ceiling installers. Younger tissue has better healing capacity, which is why early intervention in your twenties can result in full recovery. But the injury itself happens regardless of age whenever load exceeds the tissue's repair capacity over time.
▸ What's the fastest realistic recovery at each stage?
Stage 1 with immediate load reduction and decompression work: 7–14 days to pain-free. Stage 2 bursitis with physio 2x/week and proper load modification: 4–8 weeks. Stage 3 partial tear with physio and possible injection: 3–5 months minimum. Stage 4 full tear with surgery: 6–12 months. In every stage, the fastest path runs through starting the right intervention immediately — not watching to see if it settles.
▸ Can bad posture cause shoulder damage even without much overhead work?
Yes. Forward head posture and rounded shoulders compress the subacromial space even at rest. When you add overhead work on top of that pre-existing structural compromise, the mechanical load is significantly worse than in someone with good thoracic posture and shoulder blade positioning. Workers who correct their posture — pulling scapulae back and keeping the thoracic spine mobile — show measurably lower rates of impingement at the same workload. Posture isn't cosmetic; it determines how much clearance you have before tissue gets pinched.
▸ Is there anything I can do mid-shift that actually helps?
Yes, and these are small enough to do without anyone noticing. Every 20 minutes of overhead work: drop your arms to your sides and let them hang passively for 2–3 minutes — this decompresses the bursa. Shrug your shoulders up to your ears, hold 3 seconds, and release hard — this resets trapezius tension. Roll the shoulder blade back and down before going back up. On breaks, do a doorway chest opener to reverse the forward-arm posture. None of these are a substitute for physio or load reduction, but they meaningfully slow the damage accumulation on long overhead days.
What to Do Next
Route yourself based on where you are right now:
- No pain, but doing overhead work daily: Start the arm-hang routine tonight. Read the complete physical work recovery guide and build it into your post-shift routine before pain appears.
- Post-shift ache under 4 weeks: Reduce overhead load, start posterior shoulder work, check what real recovery after physical work actually looks like.
- Pain during the shift, under 2 months: Book a physio assessment this week. Don't wait. Read the evidence on why toughing it out makes injuries worse.
- Night pain, weakness, restricted motion: Stop overhead work. Get imaging. Read about the too-late line you don't want to cross — you are approaching it.
Save This Post
Bookmark this page or share it with a coworker who keeps saying their shoulder will sort itself out. The symptom matrix and decision tree are the fastest way to identify your stage and know exactly what to do about it.
Log in to leave a comment.